Dr Salman Siddiqi, Associate at Thornaby Dental Centre, has been offering treatment with the IAS Inman Aligner since 2015. Here, a recent case is described…
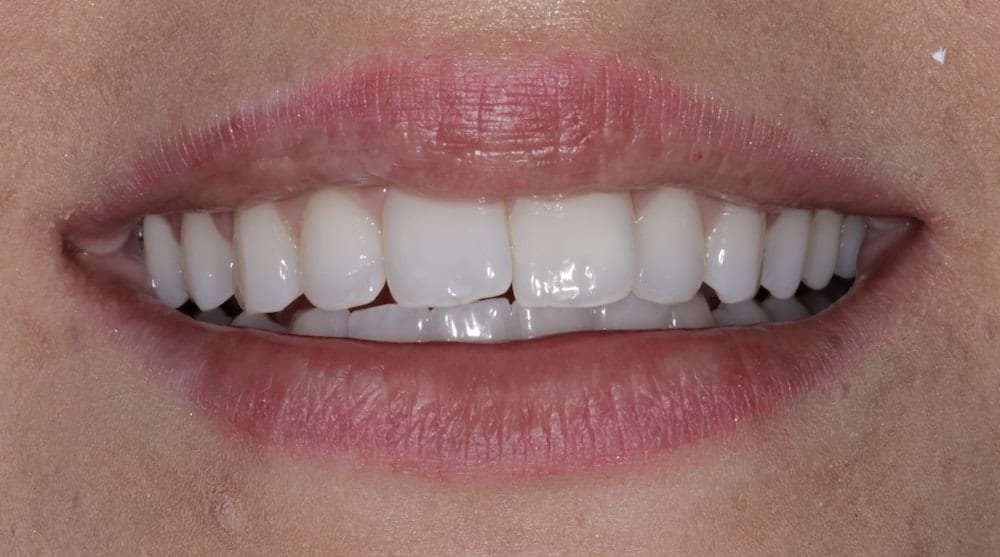
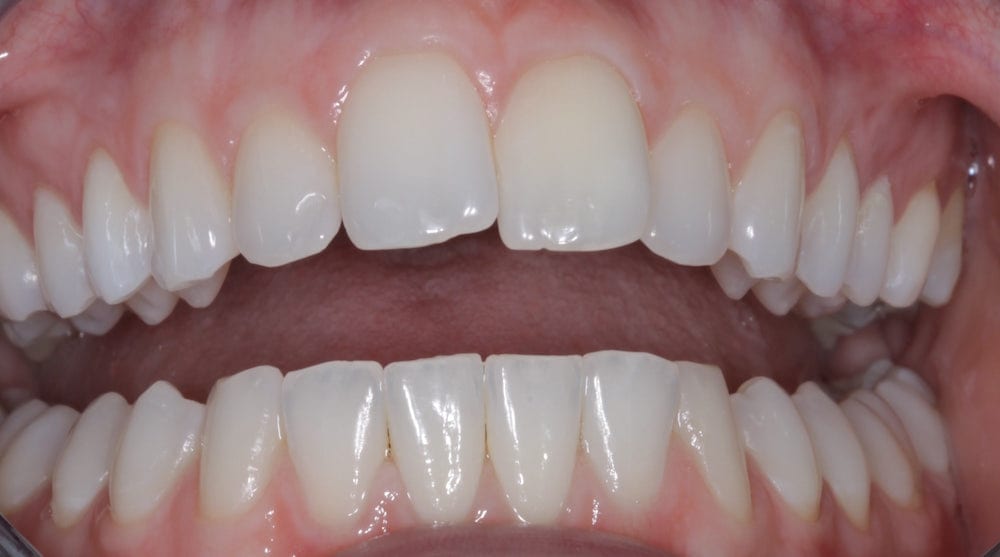
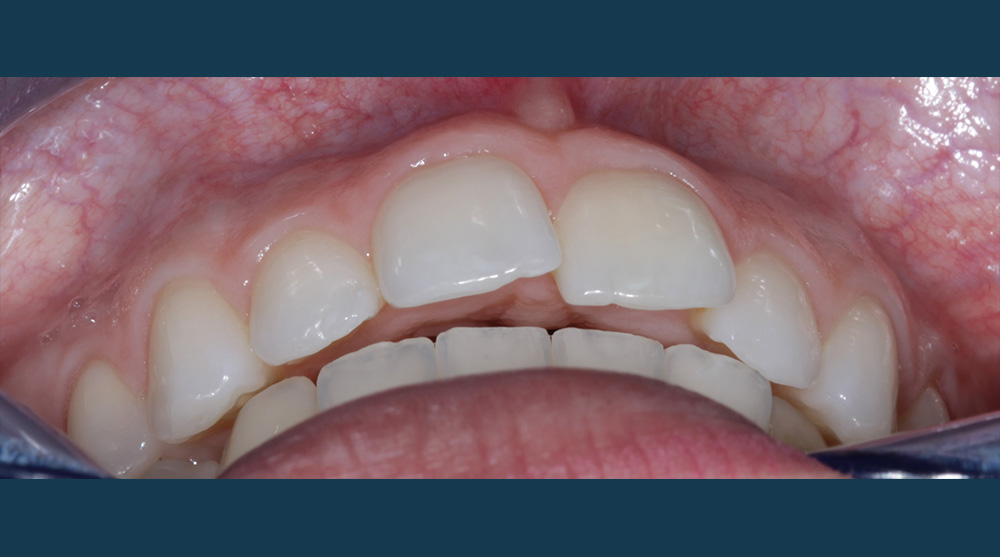
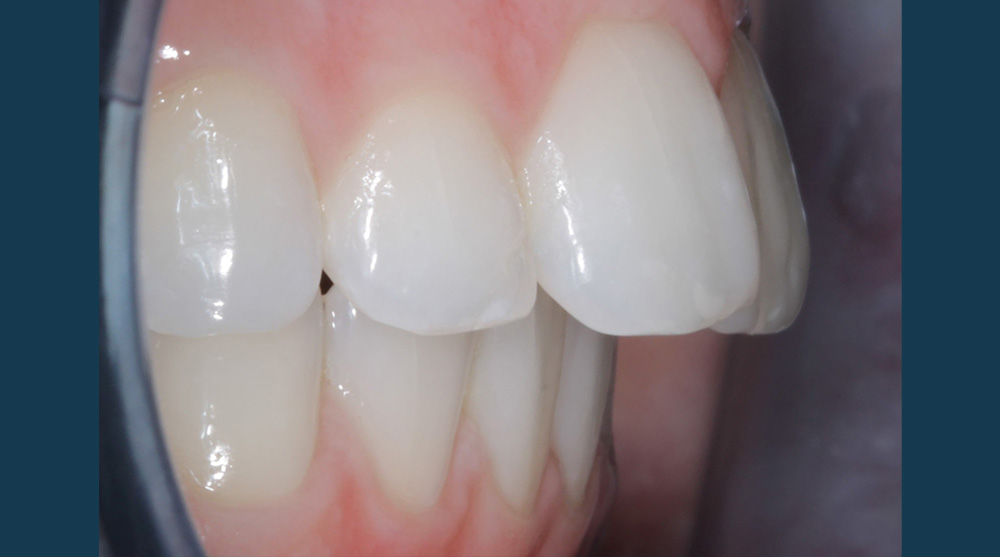
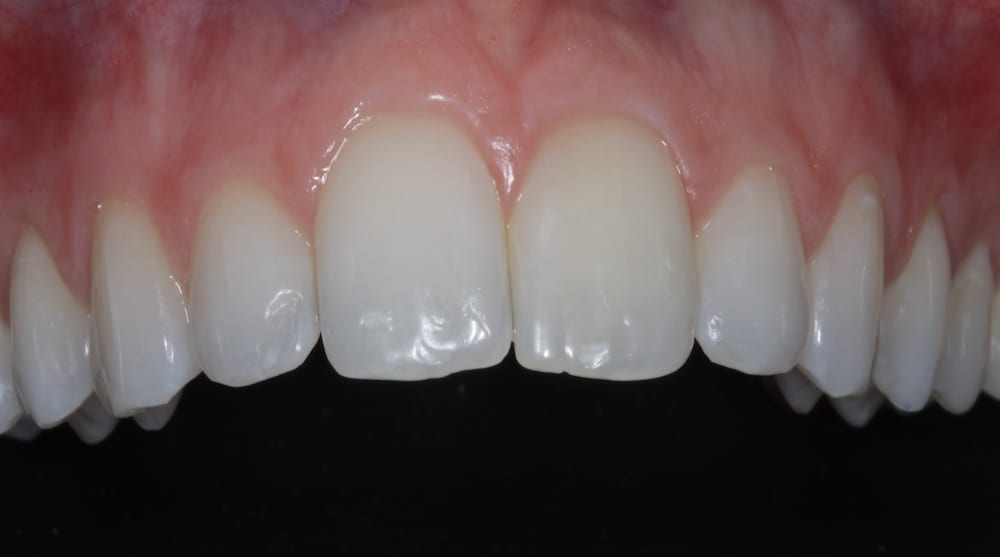
Safe, effective and minimally invasive anterior alignment is now a popular alternative to comprehensive orthodontics, especially in mild to moderate crowding cases. A prime example of this was a 21-year-old female who presented to our practice to discuss treatment options to correct the appearance of her upper anteriors – particularly her central incisors.
Patient History
The patient’s previous dental history showed that she had undergone previous upper and lower fixed orthodontics when she was 18 years old. However, following poor retention of results due to low compliance with wearing her Essix retainer, the patient experienced relapse around the upper incisors.
Examination
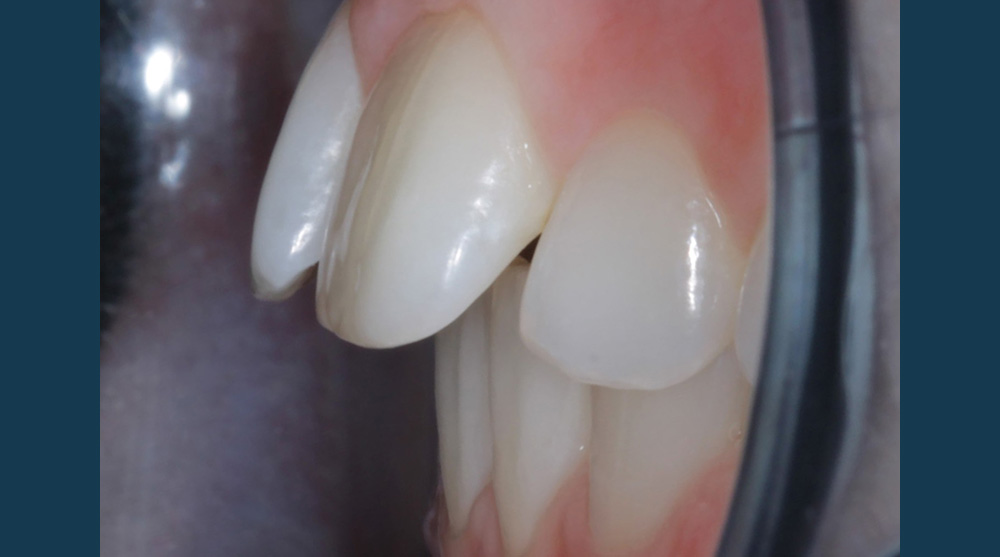
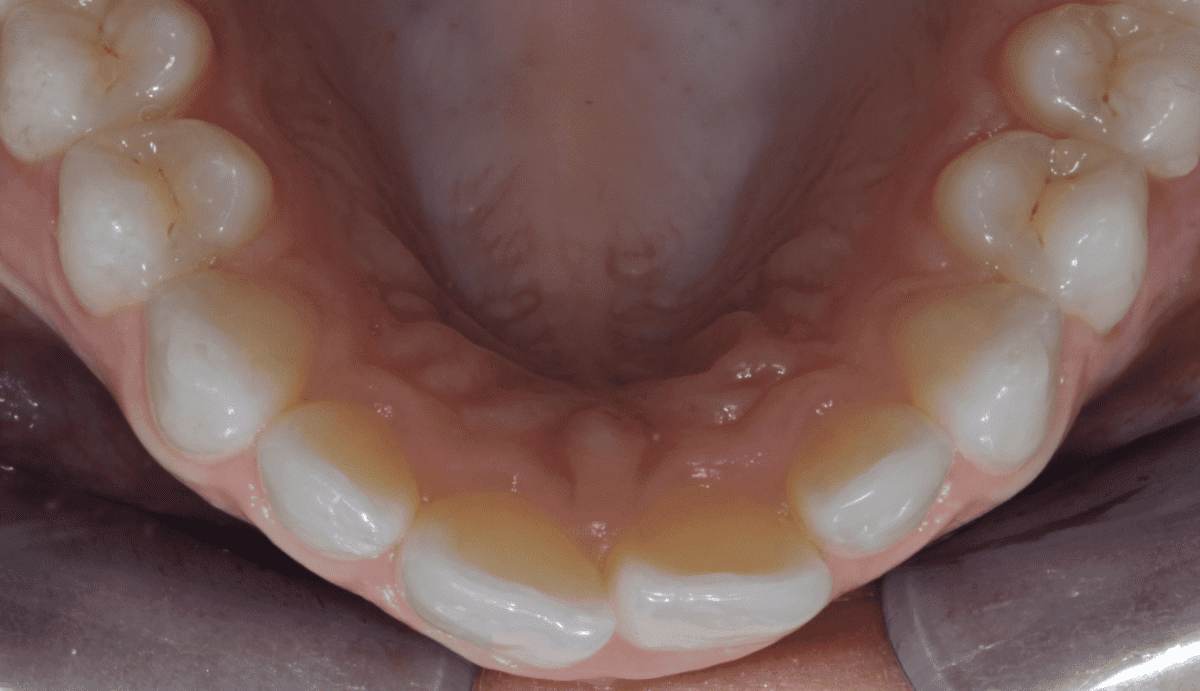
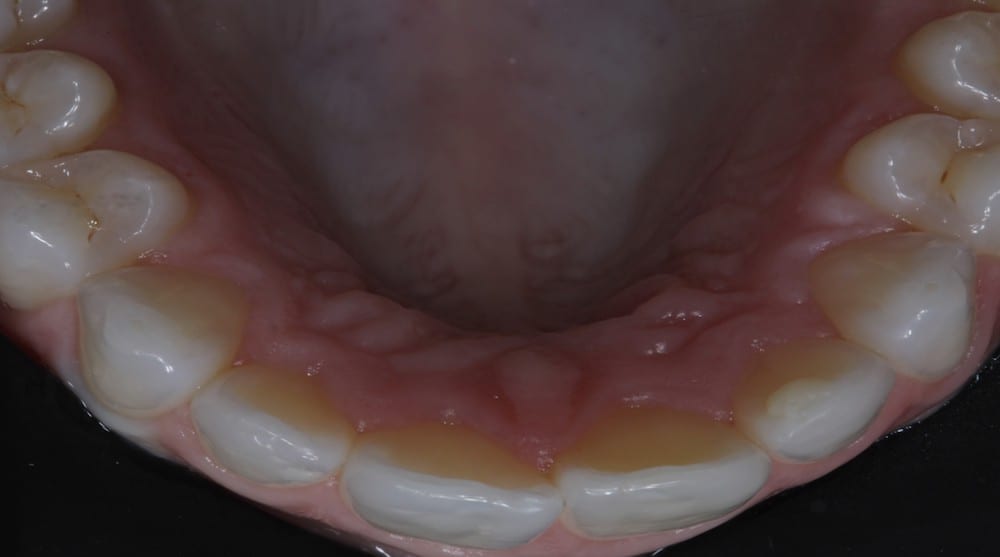
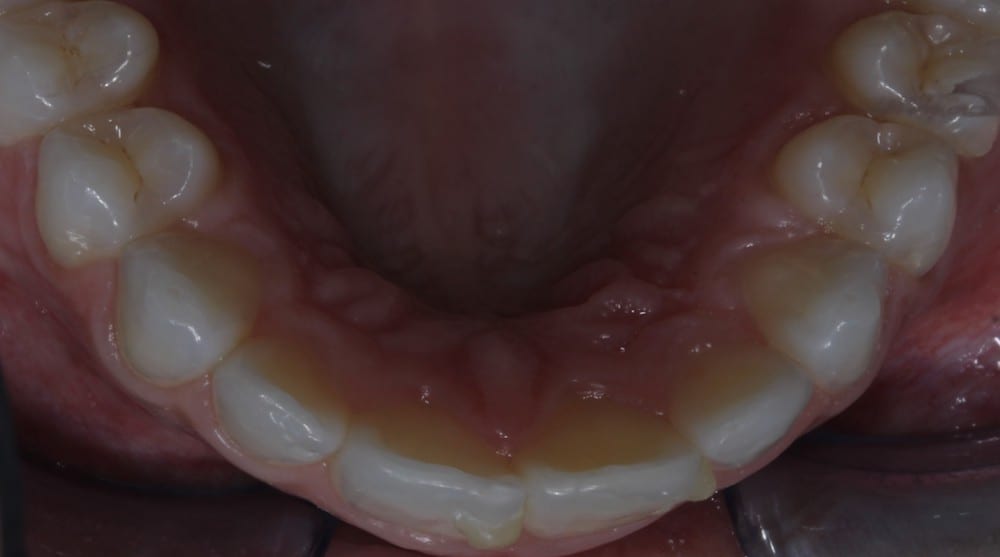
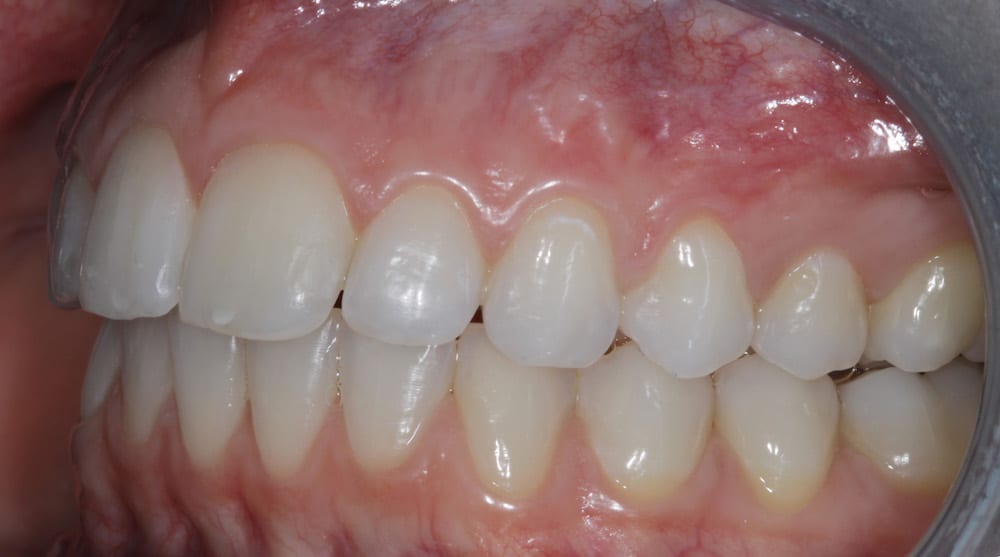
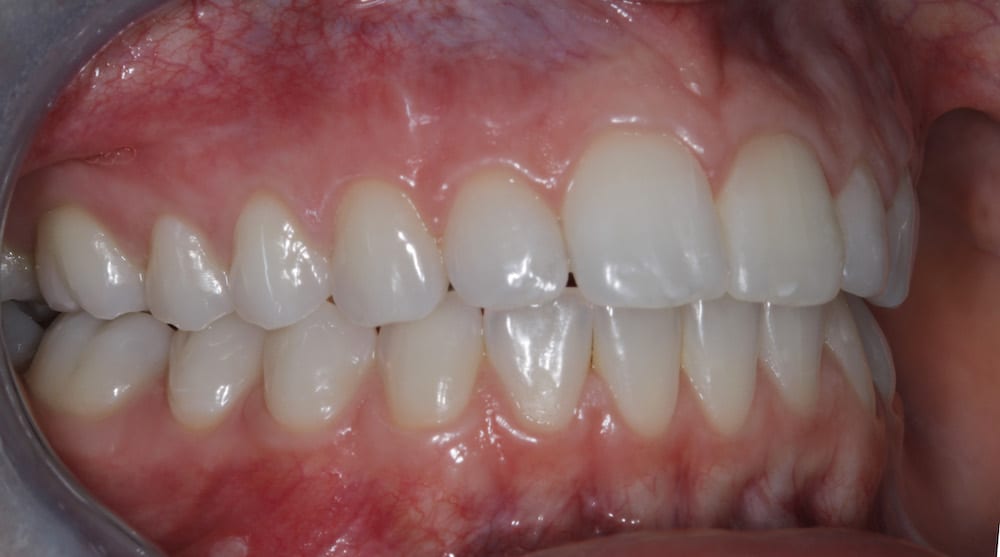
During the assessment stages a comprehensive intraoral orthodontic exam was performed. The salient features were a Class II division I malocclusion on a class II skeletal base with mild labial segment crowding, retroclined UL1 and palatally positioned UL2. Buccal segment examination revealed a bilateral Class I molar relationship with a right side Class I and left side 0.5 unit Class II canine relationship. Hard tissue examination revealed a minimally restored dentition with good oral hygiene of both smooth and interproximal surfaces.
The extra-oral examination showed competent lips at rest position and facial profile analysis revealed a low Frankfort-Mandibular Plane Angle (FMPA) and average lower face height.
A full series of intra-oral and extra-oral clinical photographs were also taken at the consultation stage as advised by the IAS assessment protocols. Digital callipers were used to accurately measure the widths of the upper anterior teeth and to calculate the degree of crowding involved.
Treatment Options
Once the treatment aims had been established, the advantages, disadvantages and risks of various treatment options were discussed with the patient, including indirect porcelain veneers, comprehensive fixed orthodontics with a specialist orthodontist or a removable appliance such as the IAS Inman Aligner. The patient was not keen on veneers due to the biological cost of removing enamel during preparation and the associated risk of devitalising the tooth in the process. Having undergone fixed brace alignment just three years previously, the patient expressed that the IAS Inman Aligner would be her preferred method of treatment – particularly as the appliance could be removed with ease during meal times and allowed some flexibility with her busy work schedule. Other advantages in comparison to fixed appliance orthodontics included the lower cost of treatment.
Pre-treatment Planning
To ensure that the aim of the treatment – which was to buccally advance the UL2 and guide mild rotations of the upper centrals – could be met with the IAS Inman Aligner, Spacewize+™ arch evaluation software was used to confirm suitability and identify a treatment plan. The Spacewize trace revealed crowding to be within 3mm and advised this case as a good candidate for the IAS Inman Aligner.
Treatment
After valid written consent was obtained, an accurate upper putty and wash impression was recorded alongside a lower opposing alginate impression and bite registration. After filling out the lab prescription with details of proposed movements, a request was made for a ‘standard’ IAS Inman Aligner. All impressions were then posted to Nimro Dental Lab in London, the authorised orthodontic lab.
The appliance was delivered after 14 days as requested and fitted at the first appointment in December 2015. The lab also provided a 3D printed model of the final treatment outcome, which was very useful in achieving patient compliance throughout the progress.
When the IAS Inman Aligner was fitted, the patient was shown how to place and remove the appliance and was instructed to wear it for at 20 hours a day. Directions were also given on cleaning and storage of the appliance.
At the fit appointment a composite anchor was placed palatally on the upper left lateral as marked on the guide model. This allowed the palatal bow to rest in the incisal third and provide the required force to labially advance the lateral.
Once the lateral was in the desired position, the palatal composite anchor was removed and labial anchors were placed on the centrals to achieve mild rotations.
The space required to achieve these movements was created using interproximal strips. The strips were passed through the required contact points as advised by the interproximal reduction (IPR) guide. Topical fluoride was applied to the surfaces all teeth where IPR was carried out.
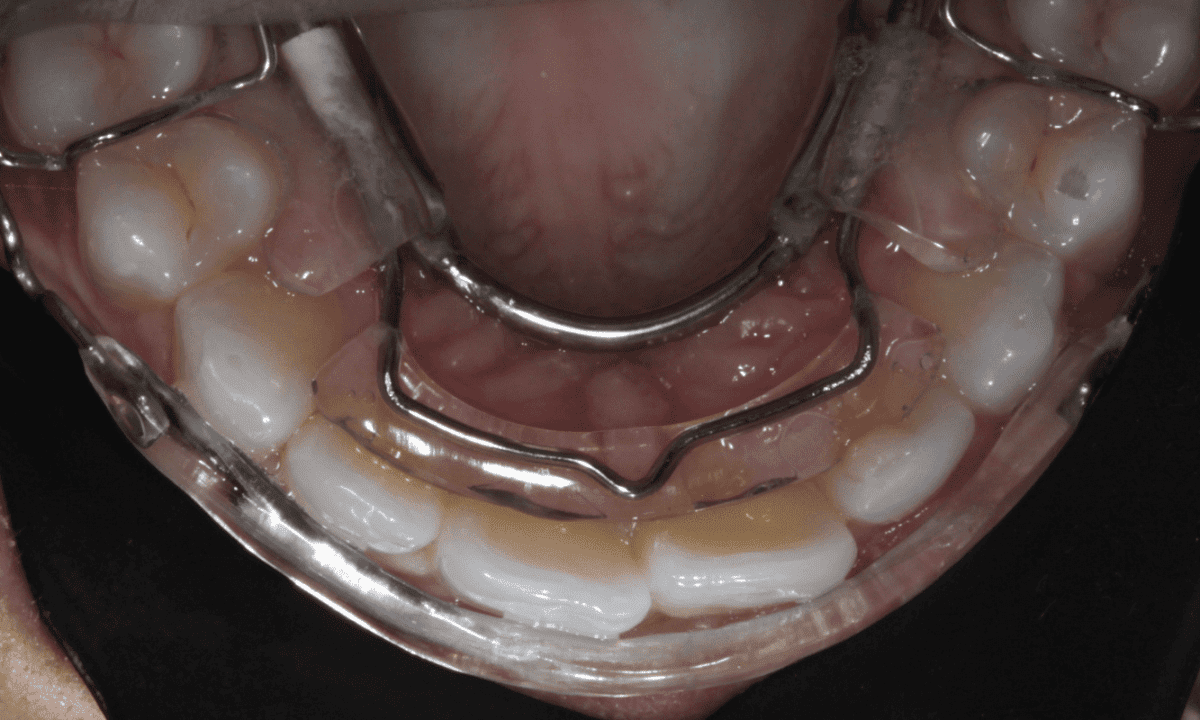
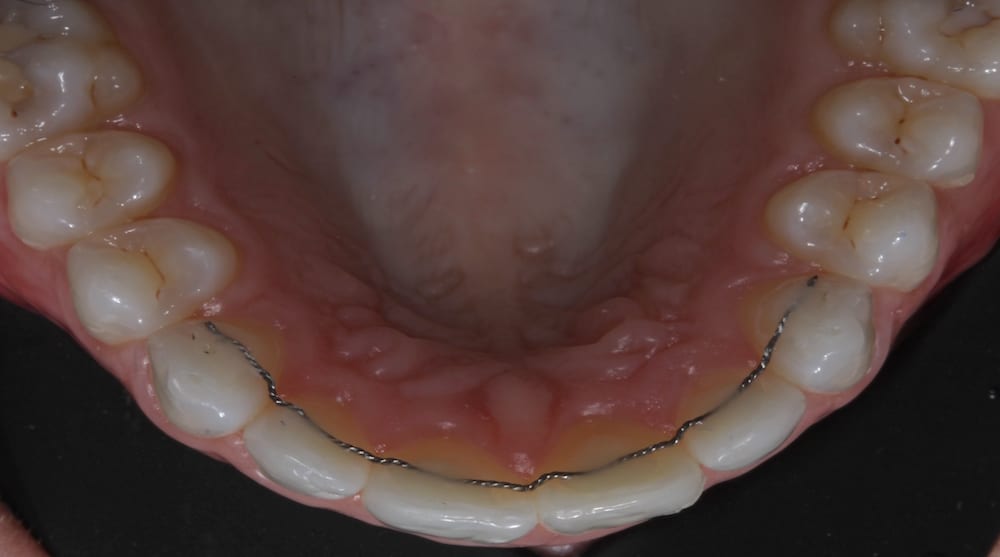
The patient was reviewed for appliance adjustment and space creation over five appointments at two weekly intervals. At the end of the treatment, a palatal wire retainer was bonded using flowable composite. Due to her dental history of orthodontic relapse the patient was also provided with a clear Essix retainer for nighttime wear in case the wire retainer debonded.
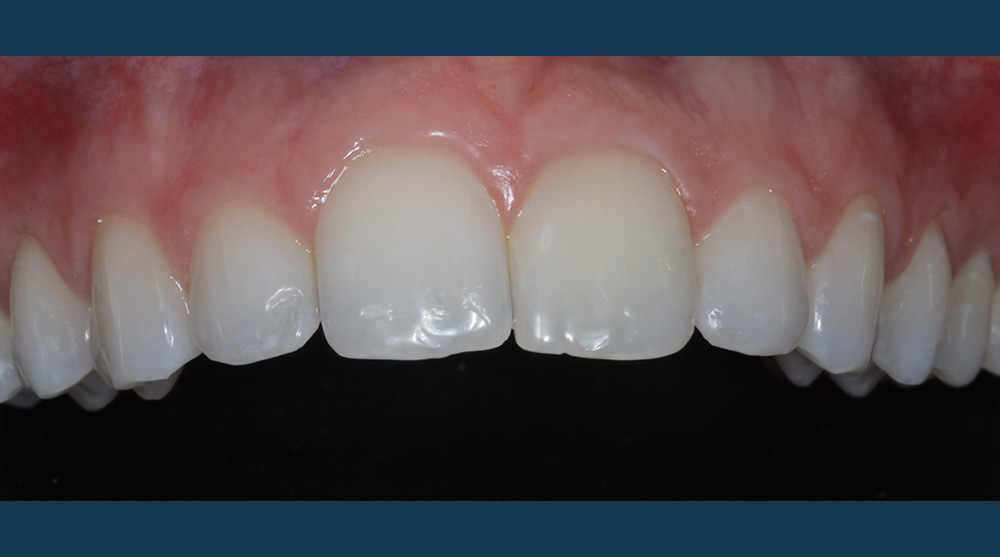
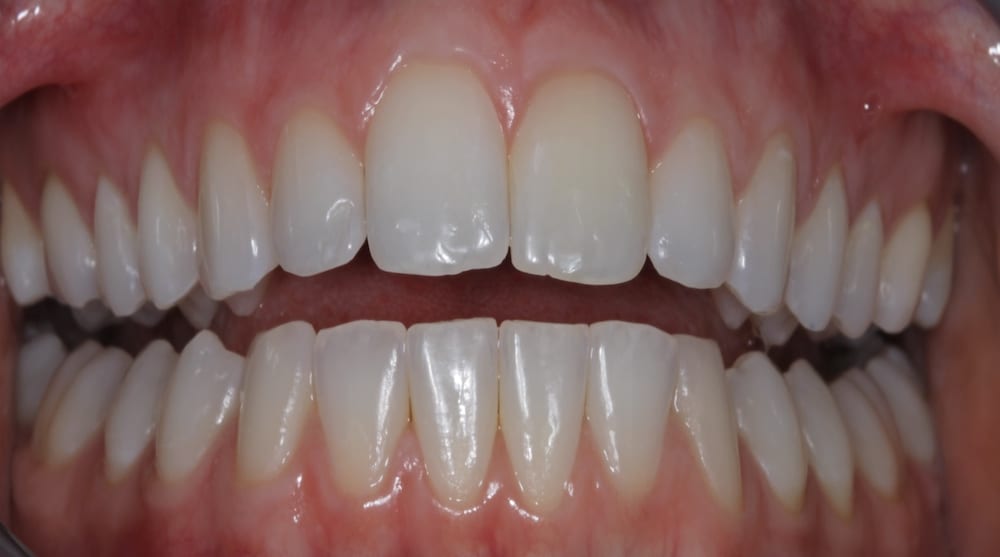
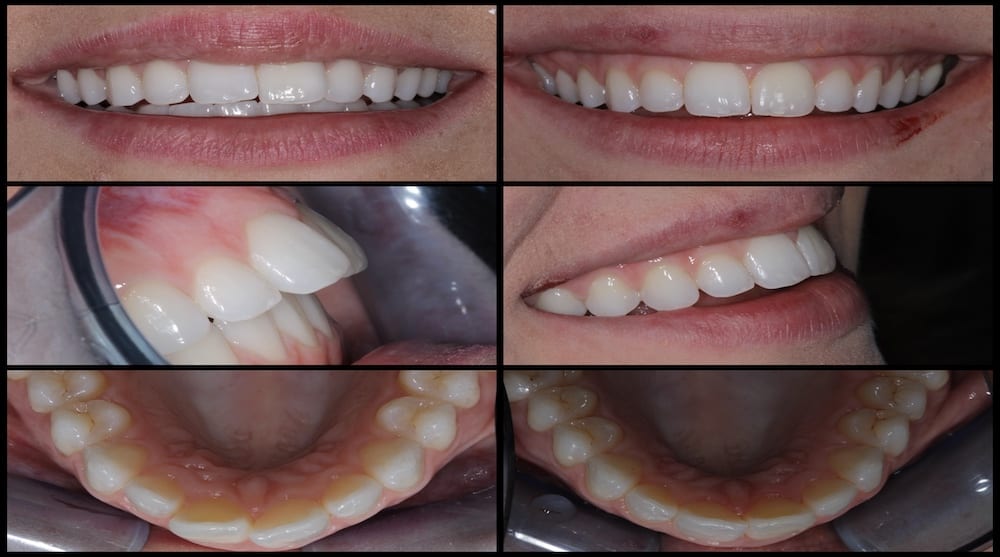
Outcome
The patient was delighted at the final result achieved. I thoroughly enjoyed treating this case and found achieving the patient’s goals using a minimally invasive treatment plan very rewarding.
The IAS Academy ethos is built on achieving predictable outcomes using sound diagnosis and treatment planning. It is using these principles that I was able to deliver the patient the results demonstrated in this case.